MERALGIA PARESTHETICA
Meralgia paresthetica is a condition attributed to entrapment or injury to the lateral femoral cutaneous nerve (LFCN) at the site where the nerve leaves the pelvis. The LFCN originates from the L2 and L3 nerve levels and is a pure sensory nerve with no motor (movement) function. The nerve exits the pelvis just medial (inside) to the anterior superior iliac spine by traversing the fibers of the inguinal ligament. Various hypotheses have been formulated for the cause of this condition including: compression of the nerve, friction against the inguinal ligament and ASIS (bony anatomy of the pelvis), or compression through ligament or muscular structures.
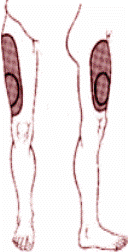
Symptoms of meralgia paresthetica may include a dull ache, itching, numbness, tingling, or burning sensation over the lateral and anterolateral thigh. The pain associated with this condition may vary in intensity from mild to very severe and frequently occurs following activity with relief following rest. If symptoms involve the lower leg or include weakness of the leg then it is highly unlikely that meralgia paresthetica is the problem.
Numerous factors may contribute to mechanical damage of the LFCN as it exits under the inguinal ligament, such as obesity, tight/constricting clothing or girdles, direct pressure on the thigh in the region of the nerve, positional alterations, or increased demands placed on the abdominal muscles secondary to pregnancy or high leg lifts. Meralgia paresthetica affects men more than women due to possible occupational considerations and may be bilateral in approximately 25 percent of individuals. Clinically, the history may reveal that the pain is potentiated by extension and relieved by flexion, as well as being aggravated by long periods of standing or walking. Physical examination may reveal a sensory loss taking the form of a reduction of tactile (touch) sensation in the distribution of the LFCN.
In diagnosing meralgia paresthetica, care should be taken to rule out intraspinal, retroperitoneal, abdominal, or pelvic pathologies, diabetes mellitus, and L3 disc prolapses. Clinically, the L3 disc prolapse may produce alteration of the patellar reflex. In contrast, the reflex will not be altered in meralgia paresthetica.
Most cases of meralgia paresthetica will respond to conservative treatment. Modalities that may prove helpful in the treatment of this condition may include ultrasound, electrical stimulation, or transverse friction techniques to break up possible adhesions affecting the LFCN at the inguinal region. Postural alterations and functional spinal problems should also be addressed in the management of this condition.
Contact Us
13710 Olive Boulevard (Primary Office)
Chesterfield, MO 63017
Telephone: 314-469-PAIN (7246)
Fax: 314-469-7251
Exchange: 314-441-6965 (for after-hour Emergencies Only)
Hours:
Monday thru Friday
8:30 AM – 4:30 PM

